A herniated disc, also referred to as a slipped or ruptured disc, affects the spine, which is a complex structure composed of vertebrae and cushioning discs. These discs facilitate movement, and they absorb daily stresses that impact the back and neck. When the gel-like interior of a disc pushes out through a tear in its tough outer layer, a herniated disc develops. Here’s information about the symptoms and treatment options for this condition:
Defining How a Disc Herniates
Every spinal disc features an outer shell called the annulus fibrosus and a pliable core known as the nucleus pulposus. A herniation occurs when the nucleus pulposus moves outward through a breach in the annulus fibrosus. This material may intrude on nearby spinal nerves, especially given the confined space within the spinal canal. This causes a range of symptoms depending on the specific nerves affected. While some refer to this as a disc slipping, the disc itself does not leave its position; the inner core projects outward.
Recognizing Herniated Disc Symptoms
A variety of symptoms may emerge depending on the disc’s location and the degree of nerve involvement. Some individuals exhibit no symptoms, and they remain unaware of the herniation. When symptoms do arise, they may affect one side of the body.
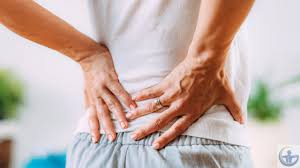
For a herniated disc in the lower back, possible symptoms include:
- Pain radiating from the lower back through the buttocks, down the leg, and sometimes reaching the foot; this is commonly described as sciatica.
- Numbness, tingling, or a pins-and-needles feeling in the leg or foot.
- Weakness in the leg that may influence the ability to lift or flex the foot.
In the neck, a herniated disc causes symptoms such as:
- Pain in the neck and shoulder, potentially traveling down the arm to the hand or fingers.
- Sensations of numbness or tingling in the shoulder, arm, or hand.
- Muscle weakness in the arm or hand.
When severe, this condition can make it difficult to walk or hold items. Symptom severity sometimes escalates with actions such as bending, twisting, coughing, or sneezing. While symptoms vary, the patterns are generally tied to the nerves impacted by the displaced disc material.
Reviewing Treatment Options
Managing a herniated disc may begin with conservative steps to ease discomfort and promote function. Some people find relief and recover over time with non-surgical options. Healthcare professionals may recommend activity modifications, such as avoiding heavy lifting or long periods of sitting.
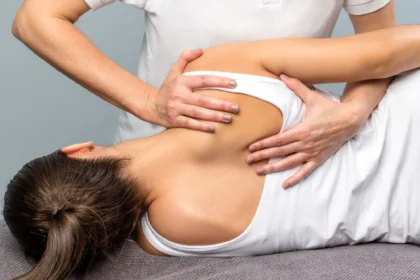
Physical therapy is a key element of many treatment plans. Therapists develop exercise regimens targeted at strengthening muscles supporting the spine, enhancing flexibility, and reducing nerve pressure. Over-the-counter medications, such as pain relievers and anti-inflammatories, are also helpful for some individuals.
When these conservative techniques provide limited relief, healthcare professionals may contemplate other solutions. Epidural steroid injections involve delivering medication near the affected nerve, and they are useful for reducing inflammation. If severe or lasting symptoms persist, surgical intervention becomes a potential next step. Surgery involves removing the part of the disc pressing on the nerve while preserving the disc’s remaining structure.
Find a Chronic Pain Specialist
A herniated disc describes the movement of the disc’s inner core through its tougher shell, often leading to nerve involvement and specific symptoms. Key signs depend on which spinal area is involved, but pain, numbness, and weakness are common. Treatment approaches emphasize physical therapy and lifestyle adjustments before further interventions, such as minimally invasive surgery. If you experience symptoms that suggest a herniated disc, contact a chronic pain specialist for assessment and advice tailored to your needs.
- Tips for Maintaining Spinal Health Through Chiropractic Care
- How to Choose the Right Sports Medicine Specialist for Your Needs
- The Connection Between Hair Loss Treatment and Overall Scalp Health
- What to Expect in a Session with a PTSD Therapist
- Exploring Ingredients and Formulations in White Label Health and Beauty Products