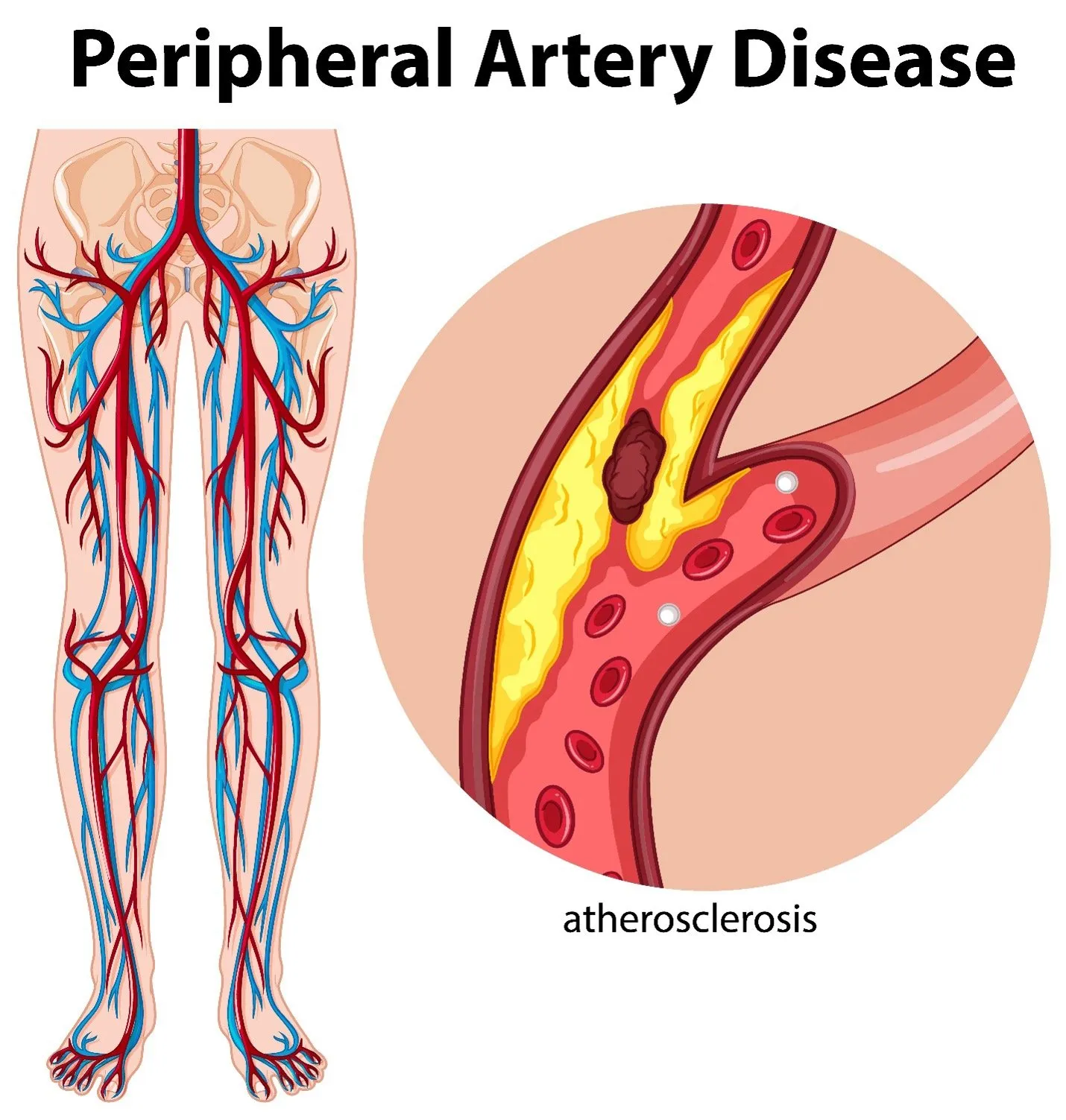
Peripheral artery disease (PAD) is a common circulatory problem and is characterized by the narrowing of arteries outside the heart and brain. When arteries become narrowed or blocked due to plaque buildup, blood flow is reduced. This can result in a range of complications, from discomfort while walking to slow-healing wounds or tissue damage. Vascular surgeons are trained to diagnose and treat disorders of the arteries and veins.
What Is Peripheral Artery Disease?
PAD occurs when fatty deposits accumulate along artery walls, particularly in arteries supplying blood to the lower extremities. These deposits narrow the vessels. Reduced circulation means that the muscles and tissues receive less blood, especially during physical activity. As demand increases with movement, a limited blood supply can trigger muscle pain or fatigue. The process of plaque accumulation is gradual and may not cause symptoms in the early stages.
How Is It Detected?
PAD symptoms range from mild to severe, and some people can remain unaware they have the condition. The most frequent early symptom is claudication, manifesting as pain, cramping, or weakness in the legs during walking or exercise. Other signs include numbness, a sense of coldness in the lower limbs, poor hair growth on the legs, slow-healing sores on the feet or toes, and color changes in the skin.
Diagnosing PAD typically starts with a review of symptoms, including a physical exam. The ankle-brachial index (ABI) is a noninvasive and widely used method that compares blood pressure in the ankles and arms. Values lower than normal suggest reduced blood flow.
How Is It Treated?
A vascular surgeon develops individualized care plans based on the severity of disease, the presence of symptoms, and overall patient health. Lifestyle changes, such as stopping smoking and managing diabetes, form the backbone of early intervention. Exercise has been shown to improve walking distance and manage symptoms for many patients.
Medications are used to manage blood pressure, cholesterol, and blood sugar levels. These aim to reduce blood clot formation and lower the risk of further arterial narrowing. When PAD is more advanced or when lifestyle changes and medication do not sufficiently improve symptoms, vascular surgeons may recommend procedures to restore blood flow.
Minimally invasive endovascular treatments such as angioplasty have become standard options for many individuals. In angioplasty, a small balloon is guided to the narrowed segment of the artery and inflated, widening the channel for blood flow. A stent may be placed to keep the artery open. Vascular surgeons provide ongoing monitoring after treatment and can address any complications. Regular assessments help detect changes in blood flow early and support wound healing in cases where tissue damage has occurred.
Meet With a Vascular Surgeon
An appointment with a vascular surgeon offers a comprehensive approach to evaluating and treating PAD. Early recognition of symptoms can prompt timely assessment and intervention. Consulting a specialist allows for a detailed circulatory evaluation and facilitates monitoring for related cardiovascular conditions. For those with risk factors, a proactive approach can support limb function and long-term vascular health. Meeting with a vascular surgeon provides a pathway to diagnosis, management, and improved quality of life for individuals living with peripheral artery disease.
- Tips for Maintaining Spinal Health Through Chiropractic Care
- How to Choose the Right Sports Medicine Specialist for Your Needs
- The Connection Between Hair Loss Treatment and Overall Scalp Health
- What to Expect in a Session with a PTSD Therapist
- Exploring Ingredients and Formulations in White Label Health and Beauty Products