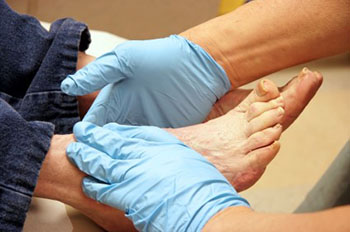
Podiatry is a specialized field of medicine dedicated to the study, diagnosis, and treatment of disorders of the foot, ankle, and lower extremities. This specialty is invaluable for diabetics, as the condition commonly leads to foot complications. Diabetic wound care focuses on preventing and managing these issues, particularly foot ulcers, to support overall health and mobility. Here are some podiatry foot care tips for diabetics:
Diabetic Podiatry Services
Podiatrists manage diabetic foot health by monitoring lower limbs, managing complications, and educating patients on preventive measures. Diabetes often causes neuropathy, or nerve damage, and circulation issues. Reduced blood flow impairs healing, especially in the legs and feet. Because of these impacts, many diabetic individuals may not feel their foot injuries, causing them to develop into ulcers.
What Are Diabetic Foot Ulcers?
Regular podiatry visits help diabetics identify potential problems before they become serious, and a podiatrist can create a personalized care plan for effective wound management. Diabetic foot ulcers are open sores or wounds that commonly develop on the bottom of the foot. These ulcers can occur in anyone with diabetes, but are more frequent in individuals who:
- Use Insulin
- Have Diabetes-related Kidney, Eye, or Heart Disease
- Are Overweight
Even a small blister or cut may develop into an ulcer if not well managed, risking the spread of infection to deeper tissues.
When Can They Occur?
Foot ulcers can result from a combination of factors. Poor circulation, high blood sugar levels, and nerve damage can make the feet vulnerable to injury. Pressure or irritation from poorly fitting shoes may also cause skin to break down, and an unnoticed cut or scrape can become infected. Ulcers may develop quickly, so daily foot inspections are a key self-care strategy.
Nonsurgical Treatments
When a diabetic foot ulcer develops, a podiatrist often begins with nonsurgical treatments to promote healing and prevent infection. After an examination, a podiatrist may start by relieving pressure on the wound and reducing pain. This is a method known as off-loading.
Other nonsurgical options include topical wound care, where special dressings and medications are applied to the ulcer to create a moist, clean healing environment. If signs of infection are present, a course of antibiotics may be prescribed to manage the bacteria. When swelling impedes circulation, compression therapy with specialized stockings or bandages may be utilized to reduce fluid buildup and support blood flow.
Surgical Treatments
If an ulcer does not respond to nonsurgical care or if the infection is severe, surgical intervention may be necessary. Surgical procedures can range from minor debridement, or removal, of infected tissue to more complex operations. A surgeon may remove infected bone or correct foot deformities, such as bunions or hammertoes, that contribute to pressure points and ulcer formation. In advanced cases where infection has spread significantly, amputation may be required to remove the affected tissue and prevent further complications.
At-home Management Strategies
Daily inspections are a fundamental way to prevent diabetic foot complications. Routinely inspect your feet and legs for any cuts, blisters, redness, or swelling, and keep your feet clean and dry. Some other at-home management strategies are:
- Wearing Properly Fitting Shoes and Socks
- Avoiding Walking Barefoot
- Maintaining Your Blood Sugar Levels
- Promoting Better Circulation With Gentle Activity
Schedule a Podiatry Appointment Today
Regular visits with a podiatrist are a proactive step in managing your diabetic foot health. A specialist can provide expert guidance, monitor for changes, and offer timely treatment to prevent serious complications. If you have diabetes, regularly scheduling a comprehensive foot examination can help you maintain your health and mobility.
- Tips for Maintaining Spinal Health Through Chiropractic Care
- How to Choose the Right Sports Medicine Specialist for Your Needs
- The Connection Between Hair Loss Treatment and Overall Scalp Health
- What to Expect in a Session with a PTSD Therapist
- Exploring Ingredients and Formulations in White Label Health and Beauty Products